POTD: Basics of Dermatology 1
This pearl will be part of a general overview of our favorite subject dermatology. It is very important to have a basic understanding of describing rashes so that our consultants (who will never come to the ED) can understand what we looking at.
(In fact, I believe dermatology only comes once or twice a week inpatient. I admitted a patient for Stevens-Johnson syndrome that didn't see a dermatologist until 3 days after admission)
Story Time – I will be sharing some of my more memorable cases that I’ve seen in relevant POTDs
This case happened during my intern year during my peds rotation.
13 yo female presenting with fever x 2 days with rash. The patient was in the ED 3-4 days ago with similar symptoms and was discharged as herpangina. The patient’s fever was intermittent (not on contiguous days) and subjective, and there were no other associated symptoms. Vital signs stable in the ED; afebrile in the ED. The patient was well appearing tolerating PO.
On her hands and feet were diffuse macular blanching erythematous undemarcated rash that were non-tender. A few of the lesions were patches about 1 x 1 cm. There were some erythematous lesions in the back of her mouth as well. The patient was discharged with a diagnosis of herpangina.
4 days later (third visit), the patient returned again but now with a bit more fatigue and the rash has gotten a bit worse. The patient was still well appearing but the macules have further progressed into patches over the hands and feet. When we re-examined the rash, underneath the blanching patches, there appeared to be non-blanching petechiae underneath. We got basic labs to rule out Kawasaki’s which were all normal and the patient was admitted; other differential included juvenile idiopathic arthritis and lupus.
The patient turned out to have Lupus.
So thinking back, if I had examined her rash more closely, I might have been able to find the petechial rash on the second visit which would have raised my concern for more systemic pathology. My takeaway is to be more thorough looking through all of the areas of rash as well as a benign patch can be covering a more concerning petechiae.
Basics of the Dermatologic exam
Take a history with OLDCARTS as one normally would with any history.
Choose a primary site and describe its morphology, size, shape, dermarcation, color, distribution. Make sure to look throughout the entire body for other lesions. Often times a patient might have an obvious primary lesion and less obvious ones in flexural surfaces can be missed; an isolated rash can be part of a systemic illness. Any associated symptoms like joint pain, abd pain, n/v/d/c, fevers/chills are key as benign appearing rashes can be a part of a more serious systemic illness.
Definitions
Morphology
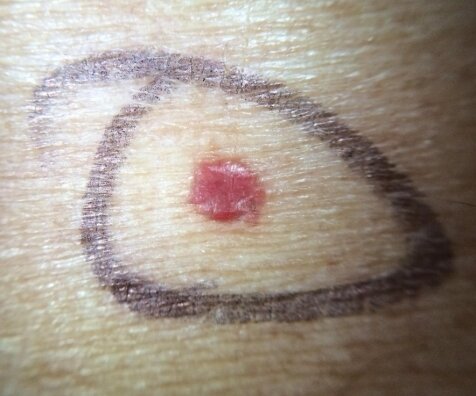
Macule: flat, nonpalpable lesion < 0.5 cm Ex: Petechiae is a form of a macule
Petechiae – small red or brown macules up to 0.5 cm that don’t blanch with pressure
Patch: flat, nonpalpable lesion > 0.5 cm Ex: vitiligo
Purpura – circumscribed petechiae more than 0.5 cm in diameter
Papule: flat, elevated, palpable lesion < 0.5 cm Ex: cherry angioma, wart
Plaque: flat, elevated area > 0.5 cm Ex. Psoriasis, seborrheic keratosis
Nodule: > 2cm dome shaped with a deep component Ex. Epidermoid cyst
Vesicle: clear fluid filled lesion < 0.5 cm Ex. Herpes, varicella
Pustule: raised fluid filled lesion < 0.5 cm filled with purulent material (similar to vesicle but with pus) Ex. Acne
Bulla: clear fluid filled lesion > 0.5 cm Ex. Bullous Pemphigoid, blister
Size
Shape
Round/discoid coin shaped, no central clearing (nummular eczema)
Oval ovoid pityriasis rosea Annular round, with active margin and central clearing (tinea corporis) Reticular net-like or lacy (lichen planus)
Linear in a line contact dermatitis Iris/target purple papule in the center of pink macule (erythema multiforme)
Serpiginous snakelike or wavy line track (cutaneous larval migrans)
Polycyclic interlocking or coalesced circles (psoriasis)
Morbilliform measles-like; maculo-papular lesions with confluence on the face and body (roseola, mononucleosis)
Demarcation: are the borders clearly defined? erysipelas vs cellulitis
Color: erythematous (cellulitis, drug reaction), loss of pigmentation (vitiligo), violaceous (Kaposi sarcoma), brown, yellow (xanthoma), black (eschar), honey-colored (impetigo)
Secondary morphology: serum/dried crust (impetigo), fissure, lichenification (thickening of skin), erosion (partial loss of epidermis), ulceration (full thickness loss of epidermis), skin sloughing
Distribution: extensor surface (psoriasis), flexor (atopic dermatitis), generalized (drug eruption), underneath belt/watch (contact dermatitis), dermatomal (varicella)
Dermatology is hard and there is an entire residency for it so we will never know everything about dermatology but there are a few can’t miss dermatologic emergencies that we can’t miss that will be covered in the next POTD!
- Kevin