I wanted to review a fairly rare but lifesaving EM procedure in neonates. This procedure is done fairly commonly in the NICU/L&D, but is done less frequently in the ED, especially with our excellent nurses who can literally get the most impossible venous accesses. If you went to Airway day, you might recall Dr. Sokolovsky describing her harrowing tale of providing neonatal resuscitation at Burning Man and performing an umbilical vein catheterization with an 18-gauge IV. Super wild! So for anyone who might find themselves in a similar poop-inducing situation with no pediatric support or NICU available, this is for you!
Umbilical vein catheterization is indicated in a neonate within 14 days post-birth requiring IV resuscitation. The stump must be "fresh", so it is most ideal in the newly born neonate. Here is an excellent video overviewing the following steps. https://pedemmorsels.com/wp-content/uploads/2019/08/UVC....mp4
Here's what you'll need:
Sterile gloves (gown and drape less non urgent)
chlorhexidine
forceps
scalpel
umbilical line (5 French is standard, 3.5 French in very premature baby)
three-way stopcock
umbilical tape of 3-0 silk/nylon
NS flush
In peds, we have umbilical vein catheterization trays located on the top shelf in Bay 31 that includes all of the above except the catheter. While the umbilical line is the traditional teaching, you can use any tube that can fit into the vein - that means an 18 gauge IV, pediatric central line, feeding tube, etc
Prep the umbilical stump
Flush the line and place
Sterilize the entire umbilical stump, including the clamp at the end of the stump, and the abdomen
Tie the umbilical tape (or a silk string) around the base of the stump loosely. This helps decreased blood flow for when the clamp is eventually removed. It can also be tightened to secure the line once placed
Holding the clamp, make a transverse cut off the stump to remove the distal tip. Cut should be made directly below the clamp or 2 cm from the abdomen.
Identifying umbilical vein and prep for insertion
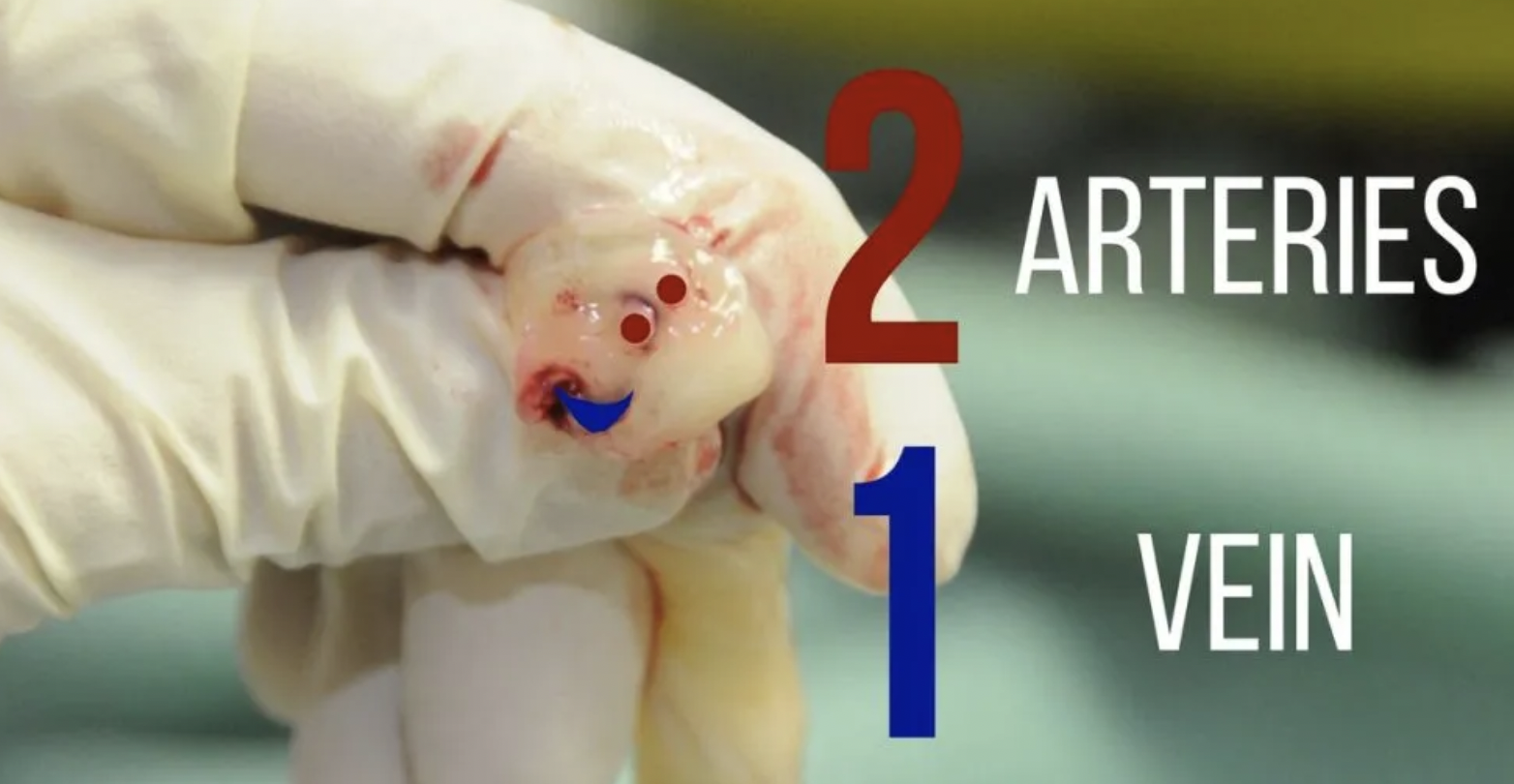
Identify the umbilical vein. The anatomy of the stump involves two smaller umbilical arteries and one umbilical vein. The arteries are typically smaller and thicker lumen, while the vein is larger and more collapsible (see below)
Remove any clots from the vein and gently dilate the vein with forceps
gently insert the line, when you get blood return insert 1-2 cm deeper, or approx 3-5 cm. If there is resistance, consider loosing the umbilical string.
Aspirate blood and flush with NS. Secure the line by tightening the umbilical string and securing with tape or purse string suture
Complications of UVC placement are similar to CVP placement: excessive bleeding, infection, thrombosis, arterial insertion. Specifically to UVC is risk of insertion too deep into the portal venous system or right atrium, which can lead to hepatic necrosis and perforation.
Resources:
https://first10em.com/umbilical-vein-catheterization/
https://wikem.org/wiki/Umbilical_vein_catheterization
https://www.ncbi.nlm.nih.gov/books/NBK549869/