Definition: definition of thrombocytopenia is a platelet count < 150 × 10E9/L
Presentation:
Often asymptomatic when first detected (significant or spontaneous bleeding rarely occurs with a platelet count > 50 × 10E9/L; 5-fold increase in risk <50 x 10E9/L)
Purpura, petechiae and bleeding from the gums and into the knee
Bleeding from venipuncture sites
Spontaneous intracerebral haemorrhage (<0.5% in ICU, higher risk if platelets <10 x 10E9/L)
Splenomegaly
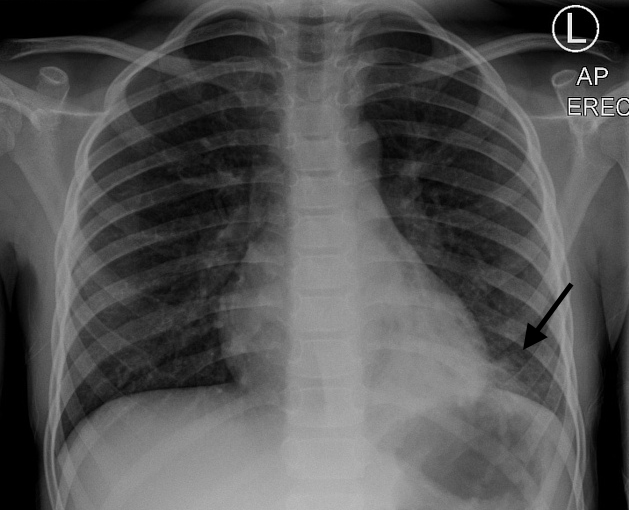
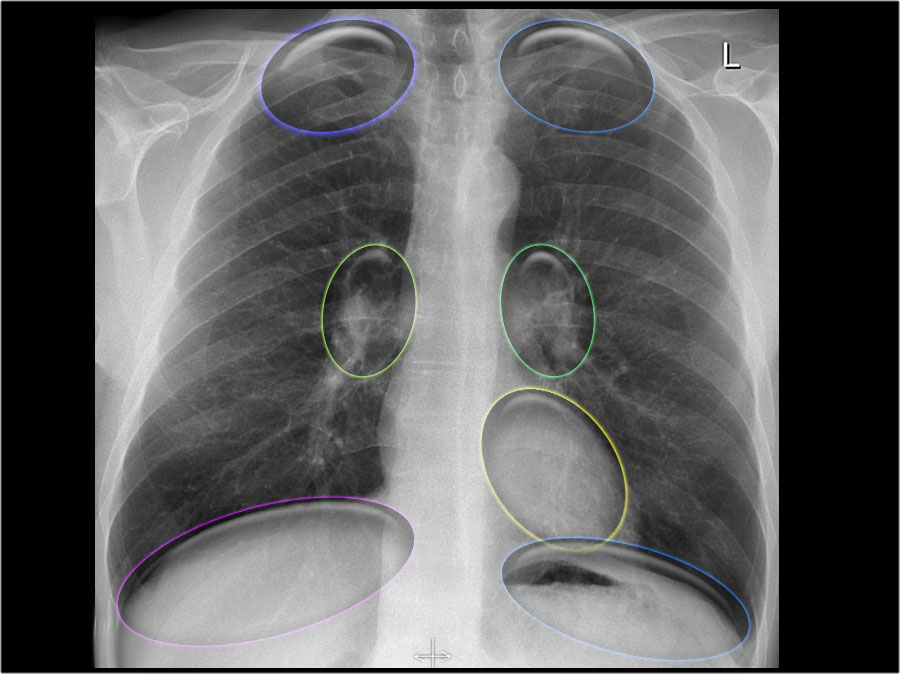
Petechiae
Purpura
Etiologies
Increased destruction
Immunologic: collagen vascular disease, infection, ITP, lymphoma/CLL, drugs (heparin, sulfonamides, aspirin, phenytoin, digoxin, vancomycin, B-lactam antibiotics)
Mechanical: TTP, HUS, DIC, chronic dialysis patient
Vasculitis
Decreased production
Decreased megakaryocytes: drugs (EtOH, thiazide, chemo, linezolid), toxins, infection, leukemia
Splenic sequestration
Dilutional
Massive transfusion, ECMO, exchange transfusion
Suggested work-up:
Repeat platelet count – Ensure value is accurate
CBC – TTP-HUS presents with anemia AND thrombocytopenia. Abnormal platelets and abnormal WBC count is concerning for primary hematologic etiology.
Peripheral smear (call the lab and ask them to add a peripheral smear) – Look for schistocytes, and also for platelet clumping to rule out pseudothrombocytopenia.
PT/PTT/INR/fibrinogen – These will be abnormal in DIC and unaffected in other etiologies.
Consult Heme/onc
Whom to consider admitting:
Severe thrombocytopenia (i.e. < 20)
Platelet count drop > 50% of baseline
Suspected leukemia, TTP-HUS, or DIC
Active bleeding
Diagnosis to consider:
HITT
Heparin-induced thrombocytopenia AND thrombosis
Use the 4T score: Timing (5-10 days after heparin exposure), degree of Thrombocytopenia (> 50% drop from baseline), no other clear etiology, and Thrombosis
If intermediate probability, send anti-platelet (PF4) antibody test
If high probability, start alternative anti-coagulation with argatroban (hepatically-cleared) or bivalirudin (renally-cleared)
ITP
Dx of exclusion
Acute => child, viral prodrome days-weeks prior, platelets <20, self-limited, supportive care unless active bleeding (steroids, IVIG, anti-Rh Ig)
Chronic => adult, no prodrome, gradual, platelets 30-100
Life-threatening bleeding: plt transfusions, steroids, IVIG
TTP-HUS
Usually idiopathic but can be 2/2 meds (clopidogrel, ticlopidine, quinine) or infection (E. coli)
Thrombocytopenia + microangiopathic hemolytic anemia (pentad of fever, anemia, thrombocytopenia, renal involvement, and neuro involvement)
Acute management is with plasmapheresis.
If not available FFP and arrange for transfer. NO PLATELETS.
Leukemia
Look for high white counts, but sometimes can present with leukopenia
Patients should be started on all-trans retinoid acid (ATRA) as soon as the diagnosis is suspected
When to transfuse platelets: <10 or <50 + active bleeding or <50 + invasive procedure. Of note: transfused platelets last 3-5 days.