Hello everyone!
For those of you who don't know me, I am Karen, a the third year resident who will be staying on as one of the ultrasound fellows next year (along with the amazing Dan Ye, who can forget his great recaps of The Pitt), I'm also one of the four chiefs following our previous admin resident and chief Kaitlyn DeStefano (whose POTDs made us laugh and cry). I have big shoes to fill with these two tough acts to follow, but I will work hard to bring fun and educational POTDs!
Continuing on The Pitt bandwagon, I love watching shows, from romances and drama, to murder mysteries and thrillers, to Kdramas and anime; I am a huge consumer of media for better or for worse. Some of my favorites are Outlander, Downton Abbey, Dark, Black Mirror, Squid Game, Attack on Titan, When Life Gives You Tangerines, of course The Pitt and so many more...
Anyways, since yesterday was the finale of HBO's "White Lotus" I wanted to talk about the Pong pong tree. (Spoilers!)
The Pong Pong tree (Cerbera odollam)—also known as the “suicide tree” is native to India and Southeast Asia. This plant contains cerberin, a cardiac glycoside similar to digoxin that disrupts cardiac activity by inhibiting the Na⁺/K⁺- ATPase pump, which can lead to fatal arrhythmias. Cerberin poisoning is difficult to detect and has been used in homicides due to its tasteless nature and delayed onset. There is no specific antidote, though digoxin-specific Fab fragments (DIGIFab) has been used.
There has been only 2 known cases of C. odollam poisoning and 1 fatality reported in the USA:
A 22-year-old pre-operative transgender man-to-woman patient ingested seeds from the Cerbera odollam tree as a suicide attempt. She presented to the emergency department with nausea, vomiting, chest pain, and dizziness approximately 7 hours after ingesting the seeds that she bought online after reading about suicide.
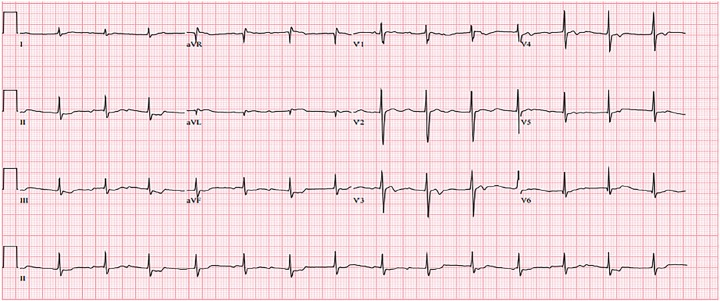
Initial electrocardiogram (ECG) showed second-degree heart block with 2:1 atrioventricular (AV) conduction and ST-segment depression with biphasic T-waves and initial serum potassium was 5.2mEq/L:
So the team administered atropine, digoxin-Fab fragments, and supportive care with improvement to sinus rhythm with first-degree AV block with persistent ST-segment depression and biphasic T-waves:
However, 2 hours later her condition deteriorated, progressing to high-degree AV block:
And subsequent cardiac arrest 30 minutes later with repeat K of 5.7mEq/L.
Despite additional doses of digoxin-specific antibody fragments (20 vials in total), lipid emulsion 20% (100 ml), right femoral CVC, and 2 hours of aggressive ACLS resuscitative efforts the patient was pronounced dead approximately 12 hours post-ingestion.
This case delineates the severe toxicity associated with C. odollam seed ingestion and highlights the challenges in managing such poisonings, even with advanced supportive measures. We should all be aware of the potential morbidity and mortality linked to this plant toxin and be prepared for aggressive resuscitative interventions.
Although the USA has only had 2 known cases of C. odollam poisoning, will a television show introducing this plant open the gates for more? Hopefully not, but as always, we will be prepared.
Misek R, Allen G, LeComte V, Mazur N. Fatality Following Intentional Ingestion of Cerbera odollam Seeds. Clin Pract Cases Emerg Med. 2018 Jun 12;2(3):223-226. doi: 10.5811/cpcem.2018.5.38345. PMID: 30083638; PMCID: PMC6075506. https://pmc.ncbi.nlm.nih.gov/articles/PMC6075506/
Karen Wong, MD
Emergency Medicine Chief Resident
KaWong@maimo.org