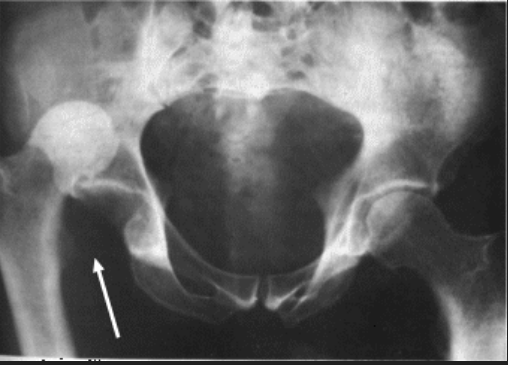
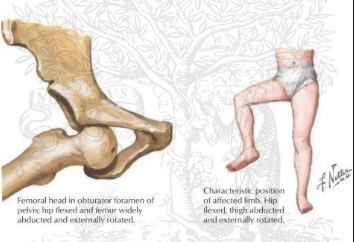
- Is a potentially lethal condition characterised by muscular rigidity and spasms, caused by the tetanospasmin toxin produced by Clostridium tetani
Types:
- cephalic
- local
- generalised
- neonatal (50% of tetanus deaths worldwide)
Tetanospasmin
- taken up by motor nerves or haematogenous spread to CNS
- preferentially prevents discharge from GABA inhibitory interneurons in spinal cord and brainstem -> unrestricted motor nerve activity and autonomic instability
Clinical features:
Clinical triad of rigidity, muscle spasms and, autonomic dysfunction
- contaminated wound or umbilical stump in neonates
- incubation period: 3-14d = time to first symptom
- rigidity (persists > 2 weeks) — trismus, dysphagia, increased tone in trunk muscles – greater on side of injury initially
- spasms (reduce after 2 weeks) — spontaneous or provoked by physical or emotional stimuli, laryngospasm, risus sardonicus, opisthotonos (severe spasm in which the back arches and the head bends back and heels flex toward the back)


- autonomic disturbance (onset after spasms, lasts 1-2 weeks) — tachycardia and hypertension may alternate with bradycardia and hypotension, dysrhythmia, cardiac arrest — salivation, bronchial secretions — gastric stasis, ileus, diarrhoea
- respiratory compromise — chest wall rigidity — laryngospasm — aspiration — retained secretions
Td Prophylaxis:
- Past vaccination unknown or <3 total
- Clean wound → Td
- Dirty wound → Td & TIG
- Past vaccination 3 or more total
- Clean wound → Td Q10yrs
- Dirty wound → Td Q5yrs
Management:
A – intubate because management requires large doses of sedatives to control muscle spasm and to overcome laryngospasm B – at risk of aspiration and have copious bronchial secretions requiring frequent suctioning, often ventilated for 2-3 weeks until spasms subside C – autonomic dysfunction requires monitoring in a critical care environment D – benzodiazepines in large doses (up to 100mg/h diazepam)
Specific Therapy:
- metronidazole (first choice); penicillin is used throughout most of the world but is a GABA antagonist
- anti-tetanus immunoglobulin: 100-300IU/kg of human Ig IM
- benzodiazepines; adjuncts include barbiturates, propofol, chlorpromazine
- Mg to 2-4mmol/L as useful in spasm treatment and limits autonomic instability
- consider dantrolene (unproven)
- clean and debride wounds (source control)
- immunize (infection does not confer immunity) – Q10 yearly
Prognosis:
Mortality >50% if untreated (usually due to respiratory failure)
Sources: Life in the fastlane, WikiEM