Happy EMS Tuesday!
We're going to slow things down from John Su's riveting email about eye emergencies to discuss the EMS protocol for “Severe Bradycardia (Pediatric)”. These are 3 words that no one wants to hear in a sentence together, so let’s get mentally prepared in case this patient comes in!
To use this protocol, patients should have: 1) HR <60 bpm, and 2) signs of shock or AMS. Any provider taking care of this type of patient can begin chest compressions and ventilations as per AHA guidelines. If an EMT is first on scene, they should immediately request ALS assistance and transport if timing makes more sense.
For paramedics, cardiac monitoring will be started and IV access will be obtained. Standing Order will allow them to perform the following:
1) Epinephrine 0.01 mg/kg (0.1mL/kg) IV of 1:10,000 concentration (max 1mg) every 3-5 minutes,
2) Atropine 0.02 mg/kg IV (min 0.1mg, max 0.5mg),
3) intubation if unable to provide effective BVM ventilations.
If that does not work, they will call OLMC for one of two options:
1) administration of a 2nd dose of Atropine 0.02 mg/kg IV
2) initiation of transcutaneous pacing. Of note, they may also for procedural sedation authorization for pediatric patients if the patient is conscious.
Check out www.nycremsco.org or the protocol binder on North Side for more.
Sincerely,
Joseph Liu, DO
Chief Resident, Emergency Medicine PGY-3
Maimonides Medical Center
- Medications
- Pharmacology
- Respiratory / Pulm
- POCUS
- Infectious Disease
- Ophthalmology
- Airway
- Obstetrics / Gynecology
- Environmental
- Procedures
- Foreign Body
- Pediatrics
- Cardiovascular
- EKG
- Critical Care
- Radiology
- Emergency
- Admin
- Orthopedics
- Nerve Blocks
- DVT
- Finance
- EMS
- Benzodiazepines
- Neurology
- Medical Legal
- Psychiatry
- Anal Fissure
- Hemorroids
- Bupivacaine
- Ropivacaine
- EM
- Neck Trauma
- Emergency Medicine
- Maisonneuve Fracture
- Diverticulitis
- Corneal Foreign Body
- Gabapentin
- Lethal Analgesic Dyad
- Opioids
- Galea Laceration
- Dialysis Catheter
- Second Victim Syndrome
- Nasal Septal Hematoma
- Nephrology / Renal
- Hematology / Oncology
- Dental / ENT
- Dermatology
- Endocrine
- Gastroenterology
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- May 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
EMS Protocol of the Week: Pediatric Respiratory Distress/Failure
Hey all,
This week's EMS protocol is on pediatric respiratory distress/failure. The thought of a pediatric patient experiencing respiratory distress is enough to cause me to go into respiratory distress... but let's discuss how our pre-hospital colleagues initiate care for these patients.
Remember that respiratory distress and respiratory failure fall on a spectrum:
Respiratory distress is characterized by:
- Increased respiratory effort/WOB
- ABSENCE of central cyanosis symptoms: anxiety, nasal flaring, increased respiratory rate, accessory muscle use (ie retractions), lethargy, etc.)
Respiratory failure is characterized by:
- Presence of central cyanosis symptoms: agitation, lethargy, severe dyspnea, labored breathing, head bobbing, grunting, severe retractions, severe bradypnea, etc.
- Hypoxia and/or hypercapnia
The prehospital approach to these kiddos corresponds to a progression of care based on the level of training present. CFRs start with ABCs and monitoring vital signs. If needed, these providers can implement airway adjuncts and administer supplemental O2 at appropriate levels for either respiratory distress or failure. At this level of training, CFRs can then address potential overdose. BLS crews will pick up from here and can additionally request ALS backup and transport the patient. If the on-scene team is ALS trained, they can perform advanced airway management if unable to continually bag ventilate the patient. From here, ALS providers will start cardiac monitoring and establish IV/IO access as necessary while en route. They can even assess and treat for a tension pneumothorax (which may develop after resuscitation has begun!).
If a known cause is identified/suspected such as aspirated foreign body or anaphylaxis, treatment via those protocols will be used. If persistence of respiratory distress/failure, then providers will default back to this protocol.
There is not a lot to be aware of from an OLMC (shameless plug for our e-mailed survey 😊) standpoint other than awareness of the level of care the on-scene providers are able to provide - this will give the receiving team a better idea of what to expect when the patient is rolled in and instill the appropriate level of fear.
See the attached protocol and check out https://nycremsco.org/ for more!Best,
Zachary KimPGY-2 Emergency Medicine
POTD: Umbilical Vein Catheterization
I wanted to review a fairly rare but lifesaving EM procedure in neonates. This procedure is done fairly commonly in the NICU/L&D, but is done less frequently in the ED, especially with our excellent nurses who can literally get the most impossible venous accesses. If you went to Airway day, you might recall Dr. Sokolovsky describing her harrowing tale of providing neonatal resuscitation at Burning Man and performing an umbilical vein catheterization with an 18-gauge IV. Super wild! So for anyone who might find themselves in a similar poop-inducing situation with no pediatric support or NICU available, this is for you!
Umbilical vein catheterization is indicated in a neonate within 14 days post-birth requiring IV resuscitation. The stump must be "fresh", so it is most ideal in the newly born neonate. Here is an excellent video overviewing the following steps. https://pedemmorsels.com/wp-content/uploads/2019/08/UVC....mp4
Here's what you'll need:
Sterile gloves (gown and drape less non urgent)
chlorhexidine
forceps
scalpel
umbilical line (5 French is standard, 3.5 French in very premature baby)
three-way stopcock
umbilical tape of 3-0 silk/nylon
NS flush
In peds, we have umbilical vein catheterization trays located on the top shelf in Bay 31 that includes all of the above except the catheter. While the umbilical line is the traditional teaching, you can use any tube that can fit into the vein - that means an 18 gauge IV, pediatric central line, feeding tube, etc
Prep the umbilical stump
Flush the line and place
Sterilize the entire umbilical stump, including the clamp at the end of the stump, and the abdomen
Tie the umbilical tape (or a silk string) around the base of the stump loosely. This helps decreased blood flow for when the clamp is eventually removed. It can also be tightened to secure the line once placed
Holding the clamp, make a transverse cut off the stump to remove the distal tip. Cut should be made directly below the clamp or 2 cm from the abdomen.
Identifying umbilical vein and prep for insertion
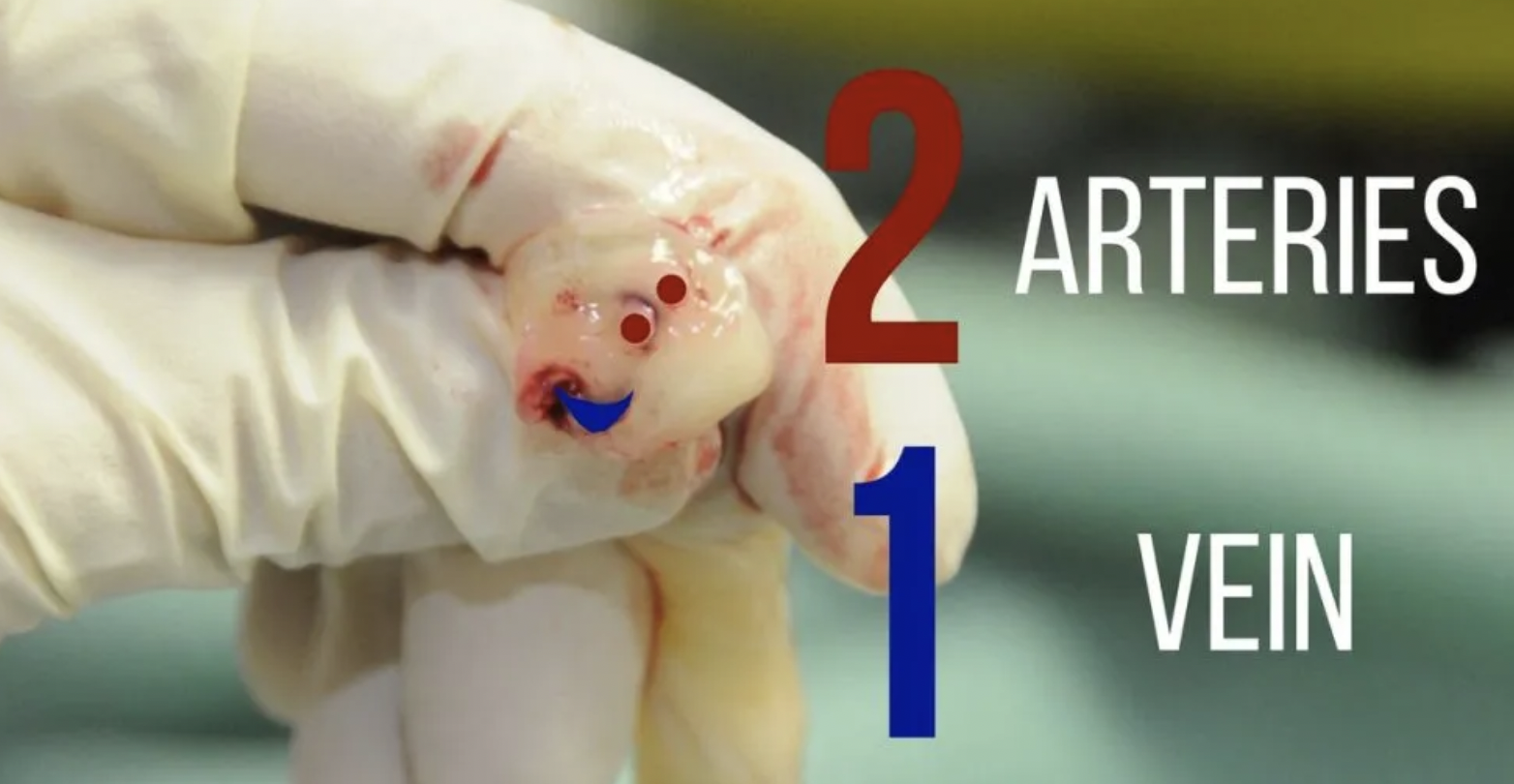
Identify the umbilical vein. The anatomy of the stump involves two smaller umbilical arteries and one umbilical vein. The arteries are typically smaller and thicker lumen, while the vein is larger and more collapsible (see below)
Remove any clots from the vein and gently dilate the vein with forceps
gently insert the line, when you get blood return insert 1-2 cm deeper, or approx 3-5 cm. If there is resistance, consider loosing the umbilical string.
Aspirate blood and flush with NS. Secure the line by tightening the umbilical string and securing with tape or purse string suture
Complications of UVC placement are similar to CVP placement: excessive bleeding, infection, thrombosis, arterial insertion. Specifically to UVC is risk of insertion too deep into the portal venous system or right atrium, which can lead to hepatic necrosis and perforation.
Resources:
https://first10em.com/umbilical-vein-catheterization/
https://wikem.org/wiki/Umbilical_vein_catheterization
https://www.ncbi.nlm.nih.gov/books/NBK549869/