>> What is it?
A well-established regional anesthetic block used for perioperative pain control of the anterior abdominal wall
Will block innervation to anterior cutaneous branches of T10 to L1 (grayed area Figure 1)
>> Block Volume: 20 - 30 mL
>> Uses in ED: Appendicitis
>> Probe Placement:
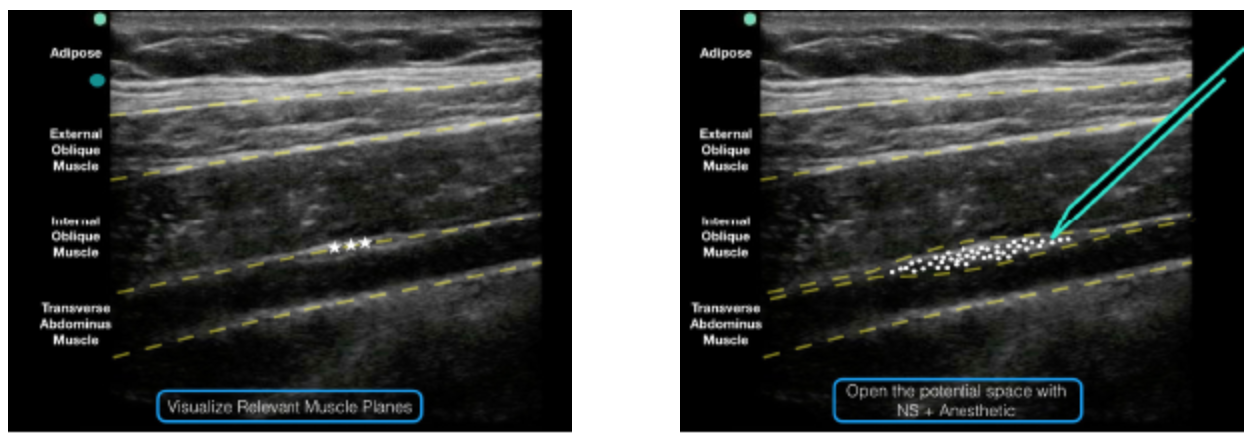
Transverse orientation above the iliac crest at the mid- to anterior-axillary line (Figures 2) so that the external oblique, internal oblique, and transversus abdominis muscle layers are easily visualized (Figure 3)
>> Approach and Needle Trajectory:
Place your patient supine and exposed from the inferior costal margin to the iliac crest
Place the needle in-plane (enter medial to lateral/posterior) and advance until the needle reaches the interfascial plane between the internal oblique and transverse abdominis muscles
Inject anesthetic. Deposition can be confirmed by visualization of anechoic fluid tracking between the internal oblique and transverse abdominis muscles (Figure 3)
Figure 1: Surface landmarks that should be palpated include the inferior costal margin and the iliac crest.
Figure 2: Place the ultrasound transducer between the inferior costal margin and iliac crest. The probe marker should point lateral/posterior.
Figure 3: Note the external oblique, internal oblique, and transverse abdominis muscles on the ultrasound screen. The goal is to deposit anesthetic in the potential space just above the transverse abdominis muscle and just below the internal oblique muscle.
Figure 4: An ultrasound representation demonstrating where anesthetic should be placed when performing a TAP block.