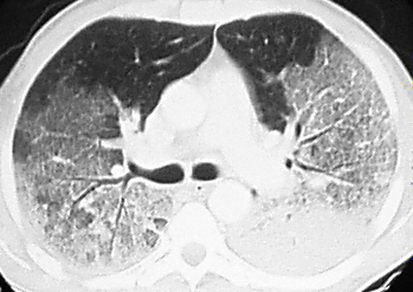
Acute respiratory distress syndrome (ARDS)
acute inflammatory lung injury that causes non-cardiogenic pulmonary edema by increasing alveolar capillary permeability.
The thickened diffusion barrier leads to hypoxemia via:
decreased lung compliance
inefficient gas exchange
Pulmonary hypertension
increased physiological dead space
Predisposing factors:
Direct lung injury: pneumonia, gastric aspiration, pulmonary contusion, near drowning, inhalation injury, transfusion-related acute lung injury
Indirect lung injury: sepsis, shock, acute pancreatitis, burns, crush injury, fat embolism, and massive transfusion
Diagnosis criteria for ARDS – Berlin definition (all 4 components must be present):
Acute onset (1 week or less)
Hypoxemia (PF ratio* < 200 mmHg with a minimum of 5 cmH2O PEEP (or CPAP))
Pulmonary edema (bilateral opacities on CXR)
Non-cardiogenic (not caused by cardiac failure)
*PF (PaO2/FiO2) ratio is the ratio of arterial oxygen partial pressure to fractional inspired oxygen. PaO2 value can be obtained from ABG, and FiO2 is 0.21 at sea level (room air) or depends on supplemental O2.
ARDS is a diagnosis of exclusion so consider first:
Cardiogenic pulmonary edema, severe multilobar pneumonia, acute exacerbation of pulmonary fibrosis, diffuse alveolar hemorrhage, idiopathic acute eosinophilic pneumonia, dissemination of lymphoma/leukemia, and several others.
Workup:
Labs: CBC, BMP, LFTs, Coags, VBG followed by ABG, troponin, BNP, lipase, consider DD
Imaging: CXR, POCUS US ECHO and CHEST and consider CT
ED Management:
Supplemental O2
Treat the underlying condition (pneumonia, sepsis, etc.)
Tempered diuresis – non-cardiogenic pulmonary edema takes much longer to respond to treatment than cardiogenic CHF, so avoid being overly aggressive with diuresis, as this may worsen underlying shock and increase likelihood of multi-organ failure
Glucocorticoids — consider steroids when ARDS precipitated by a steroid-responsive process (eg, acute eosinophilic pneumonia)
Be cautious when using non-invasive positive pressure ventilation – the benefit of NIPPV in the initial management of ARDS remains controversial.
Mostlikely patient will end up being intubated, for vent management suggested strategies are:
Use low tidal volume (6-8 mL/kg) to avoid barotrauma (ideal body weight should be calculated)
And careful FiO2:PEEP ratio titration:
ARDS severity (mortality) predictor
Mild ARDS – The PaO2/FiO2 is >200 mmHg, but ≤300 mmHg, on ventilator settings that include positive end-expiratory pressure (PEEP) or continuous positive airway pressure (CPAP) ≥5 cm H2O
Moderate ARDS – The PaO2/FiO2 is >100 mmHg, but ≤200 mmHg, on ventilator settings that include PEEP ≥5 cm H2O
Severe ARDS – The PaO2/FiO2 is ≤100 mmHg on ventilator settings that include PEEP ≥5 cm H2O.