Today we will be talking about DEEP SPACE NECK INFECTIONS , because they are doozies. Usually these get mis-triaged to SPLITFLOW, so for new 2nd years, be careful!
THE BASICS
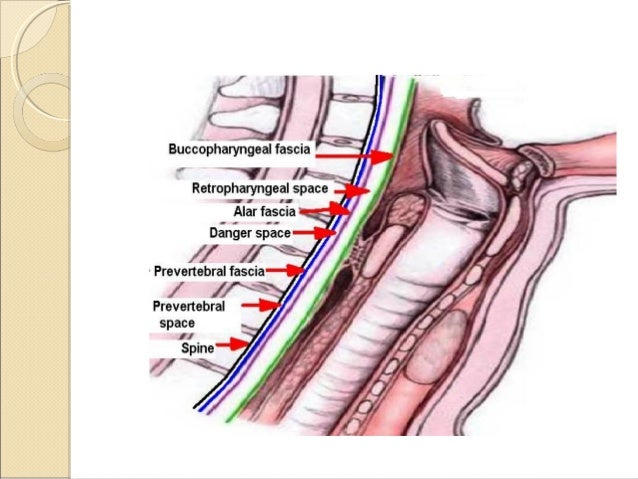
- The neck/pharynx is one of three potential spaces that can cause deep neck space infections
- retrophanygeal space
- submandibular space
- parapharyngeal space
- Usually are Polymicrobial
HOW DO THEY PRESENT??? (The starred ones are really concerning)
- Trismus *******
- Swelling below angle of mandible
- Lymphadenopathy
- Poor handling of oral secretions ******
- Asymetric pharyngeal swelling
- Odynophagia (painful swallowing)
- Muffuled voice *****
Differential?
Based on the symptoms, concern
- Peritonsillar Abscess, Retropharyngeal Abscess
- Ludwig's Angina
- Epiglottitis
- Lymphoma
- Lemierre's Syndrome
- Parapharyngeal abscess
- LIST GOES ON!!!!
BUT JOSH!?? HOW DO WE DIAGNOSE THESE????
IMAGING IMAGING IMAGING
When in doubt, get a CT with IV contrast to evaluate for deep neck space infections. However there are some signs on Neck Soft Tissue XR. Look for widening of the pre-vertebral spaces.
TREATMENT?????
AIRWAY AIRWAY AIRWAY, then maybe some ABX/Drainage
If you think that their airway is compromised, get all your airway equipment ready, monitor them, get ENT on board early, intubate early, possibly in the OR with ENT.
TAKEAWAY POINTS:
If you have someone in SPLIT with muffled voice, 1 finger trismus, with difficulty swallowing these patients, upgrade them immediately, watch their airway, get imaging and consultants on board early, and DON'T PANIC (or do.....)

